 “Cannabidiol is increasingly considered for treatment of a wide range of medical conditions. Binding studies suggest that cannabidiol binds to CB1 receptors. In the rat isolated vas deferens bioassay, a single electrical pulse causes a biphasic contraction from nerve-released ATP and noradrenaline. WIN 55,212-2 acts on prejunctional CB1 receptors to inhibit release of these transmitters. In this bioassay, we tested whether cannabidiol and SR141716 were acting as competitive antagonists of this receptor. Monophasic contractions mediated by ATP or noradrenaline in the presence of prazosin or NF449 (P2X1 inhibitor), respectively, were measured to a single electrical pulse delivered every 30 min. Following treatment with cannabidiol (10-100 μM) or SR141716 (0.003-10 μM), cumulative concentrations of WIN 55,212-2 (0.001-30 μM) were applied followed by a single electrical pulse. The WIN 55,212-2 concentration-contraction curve EC50 values were applied to global regression analysis to determine the pKB. The antagonist potency of cannabidiol at the CB1 receptor in the rat vas deferens bioassay matched the reported receptor binding affinity. Cannabidiol was a competitive antagonist of WIN 55,212-2 with pKB values of 5.90 when ATP was the effector transmitter and 5.29 when it was noradrenaline. Similarly, SR141716 was a competitive antagonist with pKB values of 8.39 for ATP and 7.67 for noradrenaline as the active transmitter. Cannabidiol’s low micromolar CB1 antagonist pKB values suggest that at clinical blood levels (1-3 μM) it may act as a CB1 antagonist at prejunctional neuronal sites with more potency when ATP is the effector than for noradrenaline.”
“Cannabidiol is increasingly considered for treatment of a wide range of medical conditions. Binding studies suggest that cannabidiol binds to CB1 receptors. In the rat isolated vas deferens bioassay, a single electrical pulse causes a biphasic contraction from nerve-released ATP and noradrenaline. WIN 55,212-2 acts on prejunctional CB1 receptors to inhibit release of these transmitters. In this bioassay, we tested whether cannabidiol and SR141716 were acting as competitive antagonists of this receptor. Monophasic contractions mediated by ATP or noradrenaline in the presence of prazosin or NF449 (P2X1 inhibitor), respectively, were measured to a single electrical pulse delivered every 30 min. Following treatment with cannabidiol (10-100 μM) or SR141716 (0.003-10 μM), cumulative concentrations of WIN 55,212-2 (0.001-30 μM) were applied followed by a single electrical pulse. The WIN 55,212-2 concentration-contraction curve EC50 values were applied to global regression analysis to determine the pKB. The antagonist potency of cannabidiol at the CB1 receptor in the rat vas deferens bioassay matched the reported receptor binding affinity. Cannabidiol was a competitive antagonist of WIN 55,212-2 with pKB values of 5.90 when ATP was the effector transmitter and 5.29 when it was noradrenaline. Similarly, SR141716 was a competitive antagonist with pKB values of 8.39 for ATP and 7.67 for noradrenaline as the active transmitter. Cannabidiol’s low micromolar CB1 antagonist pKB values suggest that at clinical blood levels (1-3 μM) it may act as a CB1 antagonist at prejunctional neuronal sites with more potency when ATP is the effector than for noradrenaline.”
https://pubmed.ncbi.nlm.nih.gov/34416240/
https://www.sciencedirect.com/science/article/abs/pii/S0014299921005860?via%3Dihub

 “The use of cannabis for skin diseases and hair regrowth is at the preliminary stage.
“The use of cannabis for skin diseases and hair regrowth is at the preliminary stage. “Nowadays cardiovascular diseases (CVDs) are the major causes for the reduction of the quality of life.
“Nowadays cardiovascular diseases (CVDs) are the major causes for the reduction of the quality of life. “In humans, various sites like cannabinoid receptors (CBR) having a binding affinity with cannabinoids are distributed on the surface of different cell types, where endocannabinoids (ECs) and derivatives of fatty acid can bind. The binding of these substance(s) triggers the activation of specific receptors required for various physiological functions, including pain sensation, memory, and appetite.
“In humans, various sites like cannabinoid receptors (CBR) having a binding affinity with cannabinoids are distributed on the surface of different cell types, where endocannabinoids (ECs) and derivatives of fatty acid can bind. The binding of these substance(s) triggers the activation of specific receptors required for various physiological functions, including pain sensation, memory, and appetite. 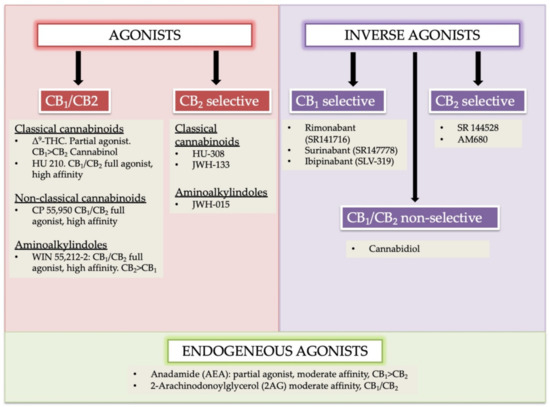
 “Chronic inflammation is considered to be a silent killer because it is the underlying cause of a wide range of clinical disorders, from cardiovascular to neurological diseases, and from cancer to obesity. In addition, there are over 80 different types of debilitating autoimmune diseases for which there are no cure. Currently, the drugs that are available to suppress chronic inflammation are either ineffective or overtly suppress the inflammation, thereby causing increased susceptibility to infections and cancer. Thus, the development of a new class of drugs that can suppress chronic inflammation is imperative.
“Chronic inflammation is considered to be a silent killer because it is the underlying cause of a wide range of clinical disorders, from cardiovascular to neurological diseases, and from cancer to obesity. In addition, there are over 80 different types of debilitating autoimmune diseases for which there are no cure. Currently, the drugs that are available to suppress chronic inflammation are either ineffective or overtly suppress the inflammation, thereby causing increased susceptibility to infections and cancer. Thus, the development of a new class of drugs that can suppress chronic inflammation is imperative. 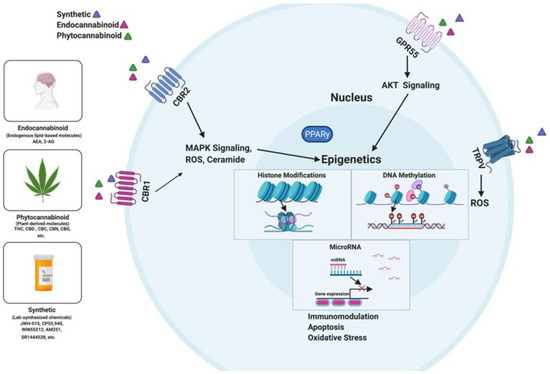
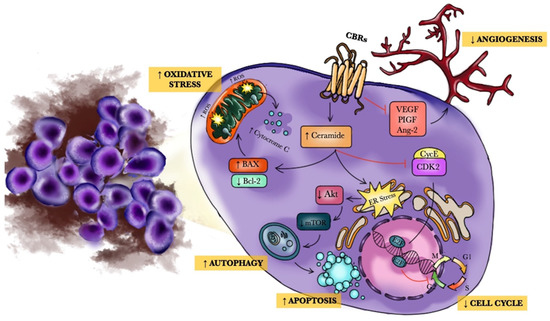
 “Human immunodeficiency virus (HIV) infection and antiretroviral therapy can independently induce HIV-associated neuropathic pain (HIV-NP).
“Human immunodeficiency virus (HIV) infection and antiretroviral therapy can independently induce HIV-associated neuropathic pain (HIV-NP). “The therapeutic potential of
“The therapeutic potential of 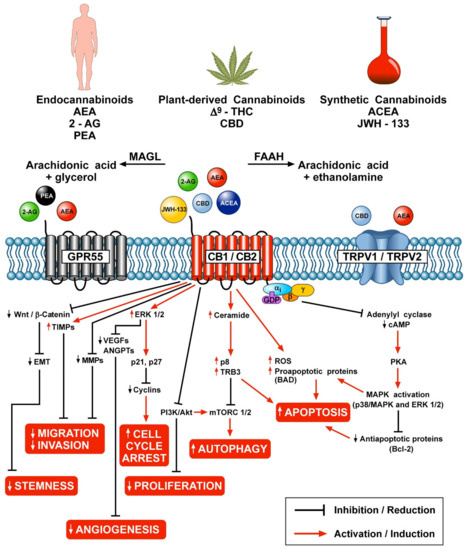
 “Venous Leg Ulcers are highly prevalent lower limb integumentary wounds that remain challenging to heal despite the use of evidence-based compression therapies. A multitude of adjuvant treatments have been studied but none have demonstrated enough efficacy to gain adoption into treatment guidelines.
“Venous Leg Ulcers are highly prevalent lower limb integumentary wounds that remain challenging to heal despite the use of evidence-based compression therapies. A multitude of adjuvant treatments have been studied but none have demonstrated enough efficacy to gain adoption into treatment guidelines.