 “The Endocannabinoid System (ECS) is primarily responsible for maintaining homeostasis, a balance in internal environment (temperature, mood, and immune system) and energy input and output in living, biological systems.
“The Endocannabinoid System (ECS) is primarily responsible for maintaining homeostasis, a balance in internal environment (temperature, mood, and immune system) and energy input and output in living, biological systems.
In addition to regulating physiological processes, the ECS directly influences anxiety, feeding behaviour/appetite, emotional behaviour, depression, nervous functions, neurogenesis, neuroprotection, reward, cognition, learning, memory, pain sensation, fertility, pregnancy, and pre-and post-natal development.
The ECS is also involved in several pathophysiological diseases such as cancer, cardiovascular diseases, and neurodegenerative diseases. In recent years, genetic and pharmacological manipulation of the ECS has gained significant interest in medicine, research, and drug discovery and development.
The distribution of the components of the ECS system throughout the body, and the physiological/pathophysiological role of the ECS-signalling pathways in many diseases, all offer promising opportunities for the development of novel cannabinergic, cannabimimetic, and cannabinoid-based therapeutic drugs that genetically or pharmacologically modulate the ECS via inhibition of metabolic pathways and/or agonism or antagonism of the receptors of the ECS. This modulation results in the differential expression/activity of the components of the ECS that may be beneficial in the treatment of a number of diseases.
This manuscript in-depth review will investigate the potential of the ECS in the treatment of various diseases, and to put forth the suggestion that many of these secondary metabolites of Cannabis sativa L. (hereafter referred to as “C. sativa L.” or “medical cannabis”), may also have potential as lead compounds in the development of cannabinoid-based pharmaceuticals for a variety of diseases.”
https://www.mdpi.com/1422-0067/22/17/9472

 “In this study cannabidiol (CBD) was administered orally to determine its effects and mechanisms in the experimental autoimmune encephalomyelitis (EAE) model of multiple sclerosis (MS). We hypothesized that 75 mg/kg of oral CBD given for 5 days after initiation of disease would reduce EAE severity through suppression of either the early peripheral immune or late neuroimmune response.
“In this study cannabidiol (CBD) was administered orally to determine its effects and mechanisms in the experimental autoimmune encephalomyelitis (EAE) model of multiple sclerosis (MS). We hypothesized that 75 mg/kg of oral CBD given for 5 days after initiation of disease would reduce EAE severity through suppression of either the early peripheral immune or late neuroimmune response.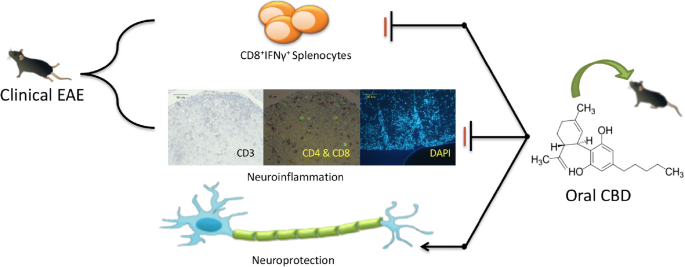
 “The consistency, efficacy, and safety of cannabis-based medicines have been demonstrated in humans, leading to the approval of the first cannabis-based therapy to alleviate spasticity and pain associated with multiple sclerosis (MS). Indeed, the evidence supporting the therapeutic potential of
“The consistency, efficacy, and safety of cannabis-based medicines have been demonstrated in humans, leading to the approval of the first cannabis-based therapy to alleviate spasticity and pain associated with multiple sclerosis (MS). Indeed, the evidence supporting the therapeutic potential of  “Cannabidiol (CBD) has been shown by our laboratory to attenuate experimental autoimmune encephalomyelitis (EAE), an animal model of multiple sclerosis (MS).
“Cannabidiol (CBD) has been shown by our laboratory to attenuate experimental autoimmune encephalomyelitis (EAE), an animal model of multiple sclerosis (MS). “T helper (Th)-17 mediate inflammation in both peripheral tissues and the central nervous system. Signal transducer and activator of transcription factor3 (STAT3) is required for Th-cell pathogenicity and its activation in the brain has been demonstrated during the acute phase of experimental autoimmune encephalomyelitis (EAE) through the mammalian target of rapamycin (mTOR) signaling. Rapamycin (RAPA), an inhibitor of mTOR, can drive Forkhead box P3 (FOXP3+) induction as a regulatory factor.
“T helper (Th)-17 mediate inflammation in both peripheral tissues and the central nervous system. Signal transducer and activator of transcription factor3 (STAT3) is required for Th-cell pathogenicity and its activation in the brain has been demonstrated during the acute phase of experimental autoimmune encephalomyelitis (EAE) through the mammalian target of rapamycin (mTOR) signaling. Rapamycin (RAPA), an inhibitor of mTOR, can drive Forkhead box P3 (FOXP3+) induction as a regulatory factor. “Multiple sclerosis (MS) is a chronic and disabling disorder of the central nervous system (CNS) characterized by neuroinflammation leading to demyelination.
“Multiple sclerosis (MS) is a chronic and disabling disorder of the central nervous system (CNS) characterized by neuroinflammation leading to demyelination. “Currently, a combination of marijuana cannabinoids including delta-9-tetrahydrocannabinol (THC) and
“Currently, a combination of marijuana cannabinoids including delta-9-tetrahydrocannabinol (THC) and  “There is a growing surge of investigative research involving the beneficial use of cannabinoids as novel interventional alternatives for multiple sclerosis (MS) and associated neuropathic pain (NPP).
“There is a growing surge of investigative research involving the beneficial use of cannabinoids as novel interventional alternatives for multiple sclerosis (MS) and associated neuropathic pain (NPP).
