“The activity of a new, terpene-based formulation, code-named NT-VRL-1, against Human Coronavirus (HCoV) strain 229E was evaluated in human lung fibroblasts (MRC-5 cells), with and without the addition of cannabidiol (CBD). The main constituents in the terpene formulation used for the experiment were beta caryophyllene, eucalyptol, and citral. The tested formulation exhibited an antiviral effect when it was pre-incubated with the host cells prior to virus infection. The combination of NT-VRL-1 with CBD potentiated the antiviral effect better than the positive controls pyrazofurin and glycyrrhizin. There was a strong correlation between the quantitative results from a cell-viability assay and the cytopathic effect seen under the microscope after 72 h. To the best of our knowledge, this is the first report of activity of a combination of terpenes and CBD against a coronavirus.”
“The activity of a new, terpene-based formulation, code-named NT-VRL-1, against Human Coronavirus (HCoV) strain 229E was evaluated in human lung fibroblasts (MRC-5 cells), with and without the addition of cannabidiol (CBD). The main constituents in the terpene formulation used for the experiment were beta caryophyllene, eucalyptol, and citral. The tested formulation exhibited an antiviral effect when it was pre-incubated with the host cells prior to virus infection. The combination of NT-VRL-1 with CBD potentiated the antiviral effect better than the positive controls pyrazofurin and glycyrrhizin. There was a strong correlation between the quantitative results from a cell-viability assay and the cytopathic effect seen under the microscope after 72 h. To the best of our knowledge, this is the first report of activity of a combination of terpenes and CBD against a coronavirus.”
Tag Archives: cannabidiol
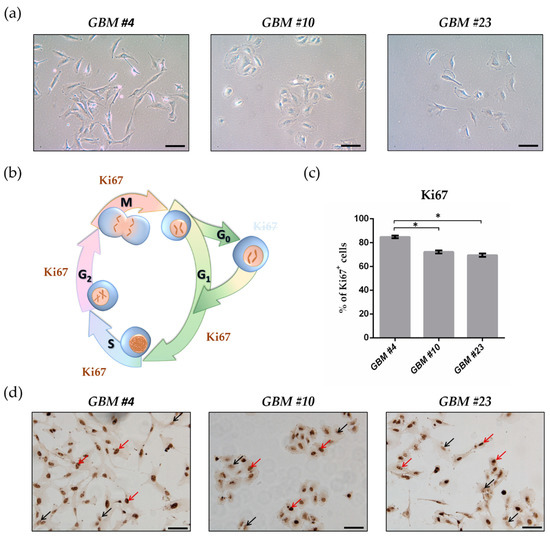
THC Reduces Ki67-Immunoreactive Cells Derived from Human Primary Glioblastoma in a GPR55-Dependent Manner

“Glioblastoma (GBM) is the most frequent malignant tumor of the central nervous system in humans with a median survival time of less than 15 months.
∆9-Tetrahydrocannabinol (THC) and cannabidiol (CBD) are the best-characterized components of Cannabis sativa plants with modulating effects on cannabinoid receptors 1 and 2 (CB1 and CB2) and on orphan receptors such as GPR18 or GPR55. Previous studies have demonstrated anti-tumorigenic effects of THC and CBD in several tumor entities including GBM, mostly mediated via CB1 or CB2.
In this study, we investigated the non-CB1/CB2 effects of THC on the cell cycle of GBM cells isolated from human tumor samples.
Cell cycle entry was measured after 24 h upon exposure by immunocytochemical analysis of Ki67 as proliferation marker. The Ki67-reducing effect of THC was abolished in the presence of CBD, whereas CBD alone did not cause any changes. To identify the responsible receptor for THC effects, we first characterized the cells regarding their expression of different cannabinoid receptors: CB1, CB2, GPR18, and GPR55. Secondly, the receptors were pharmacologically blocked by application of their selective antagonists AM281, AM630, O-1918, and CID16020046 (CID), respectively. All examined cells expressed the receptors, but only in presence of the GPR55 antagonist CID was the THC effect diminished. Stimulation with the GPR55 agonist lysophosphatidylinositol (LPI) revealed similar effects as obtained for THC. The LPI effects were also inhibited by CBD and CID, confirming a participation of GPR55 and suggesting its involvement in modifying the cell cycle of patient-derived GBM cells.”
https://pubmed.ncbi.nlm.nih.gov/33802282/
https://www.mdpi.com/2072-6694/13/5/1064
Cannabidiol Inhibits SARS-CoV-2 Replication and Promotes the Host Innate Immune Response
 “The rapid spread of COVID-19 underscores the need for new treatments.
“The rapid spread of COVID-19 underscores the need for new treatments.
Here we report that cannabidiol (CBD), a compound produced by the cannabis plant, inhibits SARS-CoV-2 infection. CBD and its metabolite, 7-OH-CBD, but not congeneric cannabinoids, potently block SARS-CoV-2 replication in lung epithelial cells.
CBD acts after cellular infection, inhibiting viral gene expression and reversing many effects of SARS-CoV-2 on host gene transcription. CBD induces interferon expression and up-regulates its antiviral signaling pathway. A cohort of human patients previously taking CBD had significantly lower SARS-CoV-2 infection incidence of up to an order of magnitude relative to matched pairs or the general population.
This study highlights CBD, and its active metabolite, 7-OH-CBD, as potential preventative agents and therapeutic treatments for SARS-CoV-2 at early stages of infection.”
https://www.biorxiv.org/content/10.1101/2021.03.10.432967v1
“Cannabis compound inhibits SARS-CoV-2 replication in human lung cells” https://www.news-medical.net/news/20210314/Cannabis-compound-inhibits-SARS-CoV-2-replication-in-human-lung-cells.aspx
A cannabidiol-loaded Mg-gallate metal-organic framework-based potential therapeutic for glioblastomas

In the present study, we explored the anticancer effect of cannabidiol loaded magnesium-gallate (CBD/Mg-GA) metal-organic framework (MOF) using the rat glioma brain cancer (C6) cell line.
Bioactive and microporous magnesium gallate MOF was employed for simultaneous delivery of two potential anticancer agents (gallic acid and CBD) to the cancer cells. Gallic acid (GA), a polyphenolic compound, is part of the MOF framework, while CBD is loaded within the framework. Slow degradation of CBD/Mg-GA MOF in physiological fluids leads to sustained release of GA and CBD.
CBD’s anti-cancer actions target mitochondria, inducing their dysfunction and generation of harmful reactive oxygen species (ROS). Anticancer effects of CBD/Mg-GA include a significant increase in ROS production and a reduction in anti-inflammatory responses as reflected by a significant decrease in TNF-α expression levels. Molecular mechanisms that underlie these effects include the modulation of NF-κB expression, triggering the apoptotic cascades of glioma cells. CBD/Mg-GA MOF has potential anti-cancer, anti-inflammatory and anti-oxidant properties.
Thus, the present study demonstrates that CBD/Mg-GA MOF may be a promising therapeutic for glioblastoma.”
https://pubmed.ncbi.nlm.nih.gov/33657198/
https://pubs.rsc.org/en/content/articlelanding/2021/TB/D0TB02780D#!divAbstract
CBD activation of TRPV1 induces oxidative signalling and subsequent ER stress in breast cancer cell lines
 “Endoplasmic reticulum (ER) stress is an imbalance between the ER’s protein-folding load and capacity. It can be induced by various physiological conditions, activating the unfolded protein response to re-establish homeostasis, promoting cell survival. Under severe or chronic stress, apoptosis is induced. Normal cells generally do not experience continuous ER stress induction. The stressful conditions experienced in the tumour microenvironment facilitates chronic ER stress and UPR activation, which plays a pivotal role in tumour survival.
“Endoplasmic reticulum (ER) stress is an imbalance between the ER’s protein-folding load and capacity. It can be induced by various physiological conditions, activating the unfolded protein response to re-establish homeostasis, promoting cell survival. Under severe or chronic stress, apoptosis is induced. Normal cells generally do not experience continuous ER stress induction. The stressful conditions experienced in the tumour microenvironment facilitates chronic ER stress and UPR activation, which plays a pivotal role in tumour survival.
Exacerbation of pre-existing ER stress can trigger cancer cell death, with a minimal effect on normal cells.
Current literature suggests that cannabinoid treatment may induce cancer cell death via ER stress; however, little is known about the mechanisms of induction.
This study proposed that cannabidiol (CBD) mechanism that occurred through the influx of Ca2+ via the TRPV1 receptor, and increasing ROS production affects protein folding and induces ER stress. ER stress was induced, and detection and quantification were completed using Thioflavin T staining and GRP78 by western blot analysis. The effect of cannabinoid treatment on ROS production and Ca2+ influx was measured. CBD was the most potent ER stress inducer, significantly increasing Ca2+ and ROS accumulation. Concomitant treatment with CBD and an antioxidant significantly increased cell viability and decreased ER stress induction in the MCF7 cell line. Concomitant treatment with a TRPV1 antagonist increased viability in this cell line.
In conclusion, the data suggested that CBD induced ER stress via Ca2+ influx through the TRPV1 receptor, thereby elevating intracellular ROS levels and disrupting protein folding.”
Cannabidiol inhibits human glioma by induction of lethal mitophagy through activating TRPV4
“Glioma is the most common primary malignant brain tumor with poor survival and limited therapeutic options. The non-psychoactive phytocannabinoid cannabidiol (CBD) has been shown to be effective against glioma; however, the molecular target and mechanism of action of CBD in glioma are poorly understood.
Here we investigated the molecular mechanisms underlying the antitumor effect of CBD in preclinical models of human glioma.
Our results showed that CBD induced autophagic rather than apoptotic cell death in glioma cells. We also showed that CBD induced mitochondrial dysfunction and lethal mitophagy arrest, leading to autophagic cell death. Mechanistically, calcium flux induced by CBD through TRPV4 (transient receptor potential cation channel subfamily V member 4) activation played a key role in mitophagy initiation. We further confirmed TRPV4 levels correlated with both tumor grade and poor survival in glioma patients. Transcriptome analysis and other results demonstrated that ER stress and the ATF4-DDIT3-TRIB3-AKT-MTOR axis downstream of TRPV4 were involved in CBD-induced mitophagy in glioma cells. Lastly, CBD and temozolomide combination therapy in patient-derived neurosphere cultures and mouse orthotopic models showed significant synergistic effect in both controlling tumor size and improving survival.
Altogether, these findings showed for the first time that the antitumor effect of CBD in glioma is caused by lethal mitophagy and identified TRPV4 as a molecular target and potential biomarker of CBD in glioma. Given the low toxicity and high tolerability of CBD, we therefore propose CBD should be tested clinically for glioma, both alone and in combination with temozolomide.”
https://pubmed.ncbi.nlm.nih.gov/33629929/
https://www.tandfonline.com/doi/abs/10.1080/15548627.2021.1885203?journalCode=kaup20
A phase 1b randomised, placebo-controlled trial of nabiximols cannabinoid oromucosal spray with temozolomide in patients with recurrent glioblastoma

Results: The most common treatment-emergent adverse events (TEAEs; both parts) were vomiting, dizziness, fatigue, nausea and headache. Most patients experienced TEAEs that were grade 2 or 3 (CTCAE). In Part 2, 33% of both nabiximols- and placebo-treated patients were progression-free at 6 months. Survival at 1 year was 83% for nabiximols- and 44% for placebo-treated patients (p = 0.042), although two patients died within the first 40 days of enrolment in the placebo arm. There were no apparent effects of nabiximols on TMZ PK.
Conclusions: With personalised dosing, nabiximols had acceptable safety and tolerability with no drug-drug interaction identified. The observed survival differences support further exploration in an adequately powered randomised controlled trial.”
Cannabigerol Is a Potential Therapeutic Agent in a Novel Combined Therapy for Glioblastoma
 “Glioblastoma is the most aggressive cancer among primary brain tumours. As with other cancers, the incidence of glioblastoma is increasing; despite modern therapies, the overall mean survival of patients post-diagnosis averages around 16 months, a figure that has not changed in many years. Cannabigerol (CBG) has only recently been reported to prevent the progression of certain carcinomas and has not yet been studied in glioblastoma. Here, we have compared the cytotoxic, apoptotic, and anti-invasive effects of the purified natural cannabinoid CBG together with CBD and THC on established differentiated glioblastoma tumour cells and glioblastoma stem cells. CBG and THC reduced the viability of both types of cells to a similar extent, whereas combining CBD with CBG was more efficient than with THC. CBD and CBG, both alone and in combination, induced caspase-dependent cell apoptosis, and there was no additive THC effect. Of note, CBG inhibited glioblastoma invasion in a similar manner to CBD and the chemotherapeutic temozolomide. We have demonstrated that THC has little added value in combined-cannabinoid glioblastoma treatment, suggesting that this psychotropic cannabinoid should be replaced with CBG in future clinical studies of glioblastoma therapy.”
“Glioblastoma is the most aggressive cancer among primary brain tumours. As with other cancers, the incidence of glioblastoma is increasing; despite modern therapies, the overall mean survival of patients post-diagnosis averages around 16 months, a figure that has not changed in many years. Cannabigerol (CBG) has only recently been reported to prevent the progression of certain carcinomas and has not yet been studied in glioblastoma. Here, we have compared the cytotoxic, apoptotic, and anti-invasive effects of the purified natural cannabinoid CBG together with CBD and THC on established differentiated glioblastoma tumour cells and glioblastoma stem cells. CBG and THC reduced the viability of both types of cells to a similar extent, whereas combining CBD with CBG was more efficient than with THC. CBD and CBG, both alone and in combination, induced caspase-dependent cell apoptosis, and there was no additive THC effect. Of note, CBG inhibited glioblastoma invasion in a similar manner to CBD and the chemotherapeutic temozolomide. We have demonstrated that THC has little added value in combined-cannabinoid glioblastoma treatment, suggesting that this psychotropic cannabinoid should be replaced with CBG in future clinical studies of glioblastoma therapy.”
https://pubmed.ncbi.nlm.nih.gov/33562819/
“Among primary brain tumours, glioblastoma is the most aggressive. As early relapses are unavoidable despite standard-of-care treatment, the cannabinoids delta-9-tetrahydrocannabinol (THC) and cannabidiol (CBD) alone or in combination have been suggested as a combined treatment strategy for glioblastomas. However, the known psychoactive effects of THC hamper its medical applications in these patients with potential cognitive impairment due to the progression of the disease. Therefore, nontoxic cannabigerol (CBG), being recently shown to exhibit anti-tumour properties in some carcinomas, is assayed here for the first time in glioblastoma with the aim to replace THC. We indeed found CBG to effectively impair the relevant hallmarks of glioblastoma progression, with comparable killing effects to THC and in addition inhibiting the invasion of glioblastoma cells. Moreover, CBG can destroy therapy-resistant glioblastoma stem cells, which are the root of cancer development and extremely resistant to various other treatments of this lethal cancer. CBG should present a new yet unexplored adjuvant treatment strategy of glioblastoma.”
Cannabis-Derived Compounds Cannabichromene and Δ9-Tetrahydrocannabinol Interact and Exhibit Cytotoxic Activity against Urothelial Cell Carcinoma Correlated with Inhibition of Cell Migration and Cytoskeleton Organization
 “Cannabis sativa contains more than 500 constituents, yet the anticancer properties of the vast majority of cannabis compounds remains unknown. We aimed to identify cannabis compounds and their combinations presenting cytotoxicity against bladder urothelial carcinoma (UC), the most common urinary system cancer.
“Cannabis sativa contains more than 500 constituents, yet the anticancer properties of the vast majority of cannabis compounds remains unknown. We aimed to identify cannabis compounds and their combinations presenting cytotoxicity against bladder urothelial carcinoma (UC), the most common urinary system cancer.
An XTT assay was used to determine cytotoxic activity of C. sativa extracts on T24 and HBT-9 cell lines. Extract chemical content was identified by high-performance liquid chromatography (HPLC). Fluorescence-activated cell sorting (FACS) was used to determine apoptosis and cell cycle, using stained F-actin and nuclei. Scratch and transwell assays were used to determine cell migration and invasion, respectively. Gene expression was determined by quantitative Polymerase chain reaction (PCR).
The most active decarboxylated extract fraction (F7) of high-cannabidiol (CBD) C. sativa was found to contain cannabichromene (CBC) and Δ9-tetrahydrocannabinol (THC). Synergistic interaction was demonstrated between CBC + THC whereas cannabinoid receptor (CB) type 1 and type 2 inverse agonists reduced cytotoxic activity.
Treatments with CBC + THC or CBD led to cell cycle arrest and cell apoptosis. CBC + THC or CBD treatments inhibited cell migration and affected F-actin integrity. Identification of active plant ingredients (API) from cannabis that induce apoptosis and affect cell migration in UC cell lines forms a basis for pre-clinical trials for UC treatment.”
Effects of cannabidiol (CBD) on the inhibition of melanoma cells in vitro
 “Cannabidiol (CBD) is one of the most popular emerging plant extracts that is being investigated for its wide range of potential health benefits.
“Cannabidiol (CBD) is one of the most popular emerging plant extracts that is being investigated for its wide range of potential health benefits.
This experiment tests how B16 mice melanoma cells, are affected by four different concentrations (0.2 mg/mL, 0.04 mg/mL, 0.008 mg/mL and 0.0016 mg/mL) of 99% CBD oil.
The results of this experiment demonstrate that CBD significantly inhibited melanoma cell growth in-vitro at 0.2 mg/mL and 0.04 mg/mL.
This shows that CBD has the potential to inhibit melanoma cell growth in vertebrates, namely mice.”
https://pubmed.ncbi.nlm.nih.gov/33428525/