 “Background and purpose: Cannabis has been used to treat epilepsy for millennia, with such use validated by regulatory approval of cannabidiol (CBD) for the treatment of Dravet syndrome. Unregulated artisanal cannabis-based products used to treat children with intractable epilepsies often contain relatively low doses of CBD but are enriched in other phytocannabinoids. This raises the possibility that other cannabis constituents might have anticonvulsant properties.
“Background and purpose: Cannabis has been used to treat epilepsy for millennia, with such use validated by regulatory approval of cannabidiol (CBD) for the treatment of Dravet syndrome. Unregulated artisanal cannabis-based products used to treat children with intractable epilepsies often contain relatively low doses of CBD but are enriched in other phytocannabinoids. This raises the possibility that other cannabis constituents might have anticonvulsant properties.
Experimental approach: We used the Scn1a+/- mouse model of Dravet syndrome to interrogate the cannabis plant for phytocannabinoids with anticonvulsant effects against hyperthermia-induced seizures. The most promising, cannabigerolic acid (CBGA), was further examined against spontaneous seizures and survival in Scn1a+/- mice. CBGA was also examined in conventional electroshock seizure models. In addition, we surveyed the pharmacological effects of CBGA across multiple drug targets.
Key results: The initial screen identified three phytocannabinoids with novel anticonvulsant properties: CBGA, cannabidivarinic acid (CBDVA) and cannabigerovarinic acid (CBGVA). CBGA was the most potent and potentiated the anticonvulsant effects of clobazam against hyperthermia-induced and spontaneous seizures, and was anticonvulsant in the MES threshold test. However, CBGA was proconvulsant in the 6-Hz threshold test and a high dose increased spontaneous seizure frequency in Scn1a+/- mice. CBGA was found to interact with numerous epilepsy-relevant targets including GPR55, TRPV1 channels and GABAA receptors.
Conclusion: These results suggest CBGA, CBDVA and CBGVA may contribute to the effects of cannabis-based products in childhood epilepsy. While these phytocannabinoids have anticonvulsant potential and could be lead compounds for drug development programs, several liabilities would need to be overcome before CBD is superseded by another in this class.”
https://bpspubs.onlinelibrary.wiley.com/doi/10.1111/bph.15661


 “Despite the high incidence of traumatic brain injury (TBI), there is no universal treatment to safely treat patients. Blunt brain injuries destroy primary neural tissue that results in impaired perfusion, excessive release of glutamate, inflammation, excitotoxicity, and progressive secondary neuronal cell death.
“Despite the high incidence of traumatic brain injury (TBI), there is no universal treatment to safely treat patients. Blunt brain injuries destroy primary neural tissue that results in impaired perfusion, excessive release of glutamate, inflammation, excitotoxicity, and progressive secondary neuronal cell death.  “Importance:
“Importance:  “Cannabis sativa
“Cannabis sativa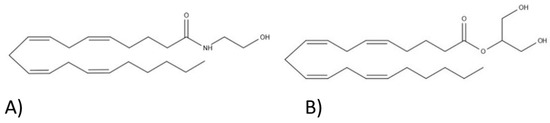
 “The Cannabis sativa plant has been used medicinally and recreationally for thousands of years, but recently only relatively some of its constituents have been identified.
“The Cannabis sativa plant has been used medicinally and recreationally for thousands of years, but recently only relatively some of its constituents have been identified. 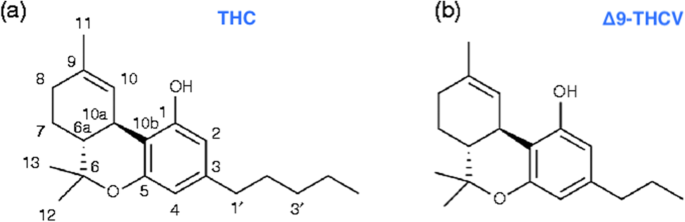 “Δ9-Tetrahydrocannabivarin (THCV) is a cannabis-derived compound with unique properties that set it apart from the more common cannabinoids, such as Δ9-tetrahydrocannabinol (THC). The main advantage of THCV over THC is the lack of psychoactive effects.
“Δ9-Tetrahydrocannabivarin (THCV) is a cannabis-derived compound with unique properties that set it apart from the more common cannabinoids, such as Δ9-tetrahydrocannabinol (THC). The main advantage of THCV over THC is the lack of psychoactive effects.  “Introduction:
“Introduction: