“Objective: Add-on cannabidiol (CBD) reduced seizures associated with Dravet syndrome (DS) in two randomized, double-blind, placebo-controlled trials: GWPCARE1 Part B (NCT02091375) and GWPCARE2 (NCT02224703). Patients who completed GWPCARE1 Part A (NCT02091206) or Part B, or GWPCARE2, were enrolled in a long-term open-label extension trial, GWPCARE5 (NCT02224573). We present an interim analysis of the safety, efficacy, and patient-reported outcomes from GWPCARE5.
Methods: Patients received a pharmaceutical formulation of highly purified CBD in oral solution (100 mg/ml), titrated from 2.5 to 20 mg/kg/day over a 2-week period, added to their existing medications. Based on response and tolerance, CBD could be reduced or increased to 30 mg/kg/day.
Results: Of the 330 patients who completed the original randomized trials, 315 (95%) enrolled in this open-label extension. Median treatment duration was 444 days (range = 18-1535), with a mean modal dose of 22 mg/kg/day; patients received a median of three concomitant antiseizure medications. Adverse events (AEs) occurred in 97% patients (mild, 23%; moderate, 50%; severe, 25%). Commonly reported AEs were diarrhea (43%), pyrexia (39%), decreased appetite (31%), and somnolence (28%). Twenty-eight (9%) patients discontinued due to AEs. Sixty-nine (22%) patients had liver transaminase elevations >3 × upper limit of normal; 84% were on concomitant valproic acid. In patients from GWPCARE1 Part B and GWPCARE2, the median reduction from baseline in monthly seizure frequency assessed in 12-week periods up to Week 156 was 45%-74% for convulsive seizures and 49%-84% for total seizures. Across all visit windows, ≥83% patients/caregivers completing a Subject/Caregiver Global Impression of Change scale reported improvement in overall condition.
Significance: We show that long-term CBD treatment had an acceptable safety profile and led to sustained, clinically meaningful reductions in seizure frequency in patients with treatment-resistant DS.”
https://pubmed.ncbi.nlm.nih.gov/34406656/
 “Cannabidiol (CBD), a primary bioactive phytocannabinoid extracted from hemp, is reported to possess potent anti-tumorigenic activity in multiple cancers.
“Cannabidiol (CBD), a primary bioactive phytocannabinoid extracted from hemp, is reported to possess potent anti-tumorigenic activity in multiple cancers. 
 “Cannabinoids, active components of the plant
“Cannabinoids, active components of the plant  “Cannabidiol (CBD), the major non-psychoactive compound found in cannabis, is frequently used both as a nutraceutical and therapeutic.
“Cannabidiol (CBD), the major non-psychoactive compound found in cannabis, is frequently used both as a nutraceutical and therapeutic.  “Clinical and preclinical evidence has indicated that estrogen depletion leads to memory impairments and increases the susceptibility to neural damage.
“Clinical and preclinical evidence has indicated that estrogen depletion leads to memory impairments and increases the susceptibility to neural damage.  “The liver is a key metabolic organ that is particularly sensitive to environmental factors, including UV radiation. As UV radiation induces oxidative stress and inflammation, natural compounds are under investigation as one method to counteract these consequences.
“The liver is a key metabolic organ that is particularly sensitive to environmental factors, including UV radiation. As UV radiation induces oxidative stress and inflammation, natural compounds are under investigation as one method to counteract these consequences.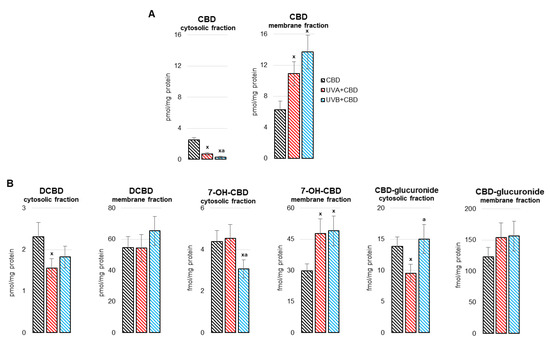
 “Obesity-related insulin resistance (IR) and attenuated brain insulin signaling are significant risk factors for neurodegenerative disorders, e.g., Alzheimer’s disease. IR and type 2 diabetes correlate with an increased concentration of sphingolipids, a class of lipids that play an essential structural role in cellular membranes and cell signaling pathways.
“Obesity-related insulin resistance (IR) and attenuated brain insulin signaling are significant risk factors for neurodegenerative disorders, e.g., Alzheimer’s disease. IR and type 2 diabetes correlate with an increased concentration of sphingolipids, a class of lipids that play an essential structural role in cellular membranes and cell signaling pathways.
 “Despite the high incidence of traumatic brain injury (TBI), there is no universal treatment to safely treat patients. Blunt brain injuries destroy primary neural tissue that results in impaired perfusion, excessive release of glutamate, inflammation, excitotoxicity, and progressive secondary neuronal cell death.
“Despite the high incidence of traumatic brain injury (TBI), there is no universal treatment to safely treat patients. Blunt brain injuries destroy primary neural tissue that results in impaired perfusion, excessive release of glutamate, inflammation, excitotoxicity, and progressive secondary neuronal cell death.  “The Cannabis sativa plant has been used medicinally and recreationally for thousands of years, but recently only relatively some of its constituents have been identified.
“The Cannabis sativa plant has been used medicinally and recreationally for thousands of years, but recently only relatively some of its constituents have been identified.