 “Cannabis is widely used in the United States with an estimated prevalence of 9.5%. Certain cannabinoids in Cannabis sativa, in particular, Δ9-tetrahydrocannabinol (THC), possess immune modulating and anti-inflammatory activity. Depending on the context, the anti-inflammatory activity of cannabinoids may be beneficial, such as in treating inflammatory diseases, or detrimental to normal immune defense against pathogens. The potential beneficial impact of cannabinoids on chronic neuroinflammation has gained recent attention. Monocyte migration to the brain has been implicated as a key event in chronic neuroinflammation and in the etiology of central nervous system diseases including viral infection (e.g., HIV-associated neurocognitive disorder). In the brain, monocytes can contribute to neuroinflammation through interactions with astrocytes, including inducing astrocyte secretion of cytokines and chemokines. In a human co-culture system, monocyte-derived IL-1β due to toll-like receptor 7 (TLR7)-activation, has been identified to promote astrocyte production of MCP-1 and IL-6. THC treatment of TLR7-stimulated co-culture suppressed monocyte secretion of IL-1β resulting in decreased astrocyte production of MCP-1 and IL-6. Furthermore, THC displayed direct inhibition of monocytes, as TLR7-stimulated monocyte monocultures treated with THC also showed suppressed IL-1β production. The cannabinoid receptor 2 (CB2) agonist, JWH-015, impaired monocyte IL-1β production similar to that of THC, suggesting THC is, in part, acting through CB2. THC also suppressed key elements of the IL-1β production pathway, including IL1B mRNA levels and caspase-1 activity. Collectively, this study demonstrates that the anti-inflammatory properties of THC suppress TLR7-induced monocyte secretion of IL-1β, through CB2, which results in decreased astrocyte secretion of MCP-1 and IL-6.
“Cannabis is widely used in the United States with an estimated prevalence of 9.5%. Certain cannabinoids in Cannabis sativa, in particular, Δ9-tetrahydrocannabinol (THC), possess immune modulating and anti-inflammatory activity. Depending on the context, the anti-inflammatory activity of cannabinoids may be beneficial, such as in treating inflammatory diseases, or detrimental to normal immune defense against pathogens. The potential beneficial impact of cannabinoids on chronic neuroinflammation has gained recent attention. Monocyte migration to the brain has been implicated as a key event in chronic neuroinflammation and in the etiology of central nervous system diseases including viral infection (e.g., HIV-associated neurocognitive disorder). In the brain, monocytes can contribute to neuroinflammation through interactions with astrocytes, including inducing astrocyte secretion of cytokines and chemokines. In a human co-culture system, monocyte-derived IL-1β due to toll-like receptor 7 (TLR7)-activation, has been identified to promote astrocyte production of MCP-1 and IL-6. THC treatment of TLR7-stimulated co-culture suppressed monocyte secretion of IL-1β resulting in decreased astrocyte production of MCP-1 and IL-6. Furthermore, THC displayed direct inhibition of monocytes, as TLR7-stimulated monocyte monocultures treated with THC also showed suppressed IL-1β production. The cannabinoid receptor 2 (CB2) agonist, JWH-015, impaired monocyte IL-1β production similar to that of THC, suggesting THC is, in part, acting through CB2. THC also suppressed key elements of the IL-1β production pathway, including IL1B mRNA levels and caspase-1 activity. Collectively, this study demonstrates that the anti-inflammatory properties of THC suppress TLR7-induced monocyte secretion of IL-1β, through CB2, which results in decreased astrocyte secretion of MCP-1 and IL-6.
SIGNIFICANCE STATEMENT: As cannabis use is highly prevalent in the United States and has putative anti-inflammatory properties, it is important to investigate the effect of cannabinoids on immune cell function. Furthermore, cannabinoids have garnered particular interest due to their potential beneficial effects on attenuating viral-induced chronic neuroinflammation. This study utilized a primary human co-culture system to demonstrate that the major psychotropic cannabinoid in cannabis, Δ9-tetrahydrocannabinol (THC) and a cannabinoid receptor-2 (CB2) selective agonist, suppress specific monocyte-mediated astrocyte inflammatory responses. In the context of viral-induced chronic neuroinflammation, the findings presented here suggest that cannabinoids via CB2 ligation may have beneficial anti-inflammatory effects.”
https://www.ncbi.nlm.nih.gov/pubmed/31383729
http://jpet.aspetjournals.org/content/early/2019/08/05/jpet.119.260661

 “As more states enact laws liberalizing marijuana use and the U.S. opioid epidemic surges to unprecedented levels, understanding the relationship between marijuana and opioids is growing increasingly important.
“As more states enact laws liberalizing marijuana use and the U.S. opioid epidemic surges to unprecedented levels, understanding the relationship between marijuana and opioids is growing increasingly important. “Δ9-tetrahydrocannabinol (Δ9-THC), the primary active component in Cannabis sativa preparations such as hashish and marijuana, signals by binding to cell surface receptors. Two types of receptors have been cloned and characterized as cannabinoid (CB) receptors. CB1 receptors (CB1R) are ubiquitously present in the central nervous
“Δ9-tetrahydrocannabinol (Δ9-THC), the primary active component in Cannabis sativa preparations such as hashish and marijuana, signals by binding to cell surface receptors. Two types of receptors have been cloned and characterized as cannabinoid (CB) receptors. CB1 receptors (CB1R) are ubiquitously present in the central nervous  “Ischemia and reperfusion of intestinal tissue (intestinal I/R) induces disruption of ileal contractility and chain responses of inflammatory.
“Ischemia and reperfusion of intestinal tissue (intestinal I/R) induces disruption of ileal contractility and chain responses of inflammatory. “Currently, a combination of marijuana cannabinoids including delta-9-tetrahydrocannabinol (THC) and
“Currently, a combination of marijuana cannabinoids including delta-9-tetrahydrocannabinol (THC) and  “Few studies have tested the hypothesis that adolescent
“Few studies have tested the hypothesis that adolescent  “Literature suggests the role of
“Literature suggests the role of  “It is well known that certain active ingredients of the plants of Cannabis genus, i.e., the “phytocannabinoids” [pCBs; e.g., (−)-trans-Δ9-tetrahydrocannabinol (THC), (−)-cannabidiol, etc.] can influence a wide array of biological processes, and the human body is able to produce endogenous analogs of these substances [“endocannabinoids” (eCB), e.g., arachidonoylethanolamine (anandamide, AEA), 2-arachidonoylglycerol (2-AG), etc.]. These ligands, together with multiple receptors (e.g., CB1 and CB2 cannabinoid receptors, etc.), and a complex enzyme and transporter apparatus involved in the synthesis and degradation of the ligands constitute the endocannabinoid system (ECS), a recently emerging regulator of several physiological processes. The ECS is widely expressed in the human body, including several members of the innate and adaptive immune system, where eCBs, as well as several pCBs were shown to deeply influence immune functions thereby regulating inflammation, autoimmunity, antitumor, as well as antipathogen immune responses, etc. Based on this knowledge, many in vitro and in vivo studies aimed at exploiting the putative therapeutic potential of cannabinoid signaling in inflammation-accompanied diseases (e.g., multiple sclerosis) or in organ transplantation, and to dissect the complex immunological effects of medical and “recreational” marijuana consumption. Thus, the objective of the current article is (i) to summarize the most recent findings of the field; (ii) to highlight the putative therapeutic potential of targeting cannabinoid signaling; (iii) to identify open questions and key challenges; and (iv) to suggest promising future directions for cannabinoid-based drug development.
“It is well known that certain active ingredients of the plants of Cannabis genus, i.e., the “phytocannabinoids” [pCBs; e.g., (−)-trans-Δ9-tetrahydrocannabinol (THC), (−)-cannabidiol, etc.] can influence a wide array of biological processes, and the human body is able to produce endogenous analogs of these substances [“endocannabinoids” (eCB), e.g., arachidonoylethanolamine (anandamide, AEA), 2-arachidonoylglycerol (2-AG), etc.]. These ligands, together with multiple receptors (e.g., CB1 and CB2 cannabinoid receptors, etc.), and a complex enzyme and transporter apparatus involved in the synthesis and degradation of the ligands constitute the endocannabinoid system (ECS), a recently emerging regulator of several physiological processes. The ECS is widely expressed in the human body, including several members of the innate and adaptive immune system, where eCBs, as well as several pCBs were shown to deeply influence immune functions thereby regulating inflammation, autoimmunity, antitumor, as well as antipathogen immune responses, etc. Based on this knowledge, many in vitro and in vivo studies aimed at exploiting the putative therapeutic potential of cannabinoid signaling in inflammation-accompanied diseases (e.g., multiple sclerosis) or in organ transplantation, and to dissect the complex immunological effects of medical and “recreational” marijuana consumption. Thus, the objective of the current article is (i) to summarize the most recent findings of the field; (ii) to highlight the putative therapeutic potential of targeting cannabinoid signaling; (iii) to identify open questions and key challenges; and (iv) to suggest promising future directions for cannabinoid-based drug development.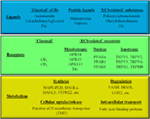
 “Our main aim was to investigate the short‐term therapeutic effects, safety/tolerability and potential side effects of the cannabis galenical preparation (Bedrocan) in patients with a range of chronic conditions unresponsive to other treatments.
“Our main aim was to investigate the short‐term therapeutic effects, safety/tolerability and potential side effects of the cannabis galenical preparation (Bedrocan) in patients with a range of chronic conditions unresponsive to other treatments.